Slow Flow – Case 2
Clinical Presentation
- 76-year-old female who presented with chest pain (CCS Class III) and was referred for staged PCI of the RCA.
Past Medical History
- HTN, HLD, Active Tobacco Use, COPD, GERD
- LVEF 60%
Clinical Variables
- Stress MPI: Small to medium anterior apical ischemia.
- Prior Cardiac Catheterization: Mid LAD 90% stenosis s/p successful PCI, mid RCA 80-90% focal stenosis, and distal RCA 70% stenosis.
Medications
- Home Medications: Aspirin, Clopidogrel, Simvastatin, Carvedilol, Valsartan, Furosemide, Dorzolamide-Timolol
- Adjunct Pharmacotherapy: Clopidogrel, Bivalirudin
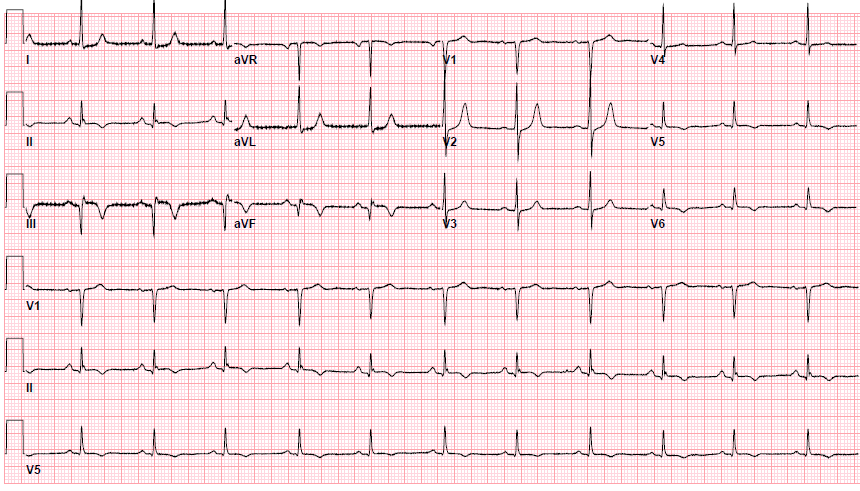
Pre-procedure EKG
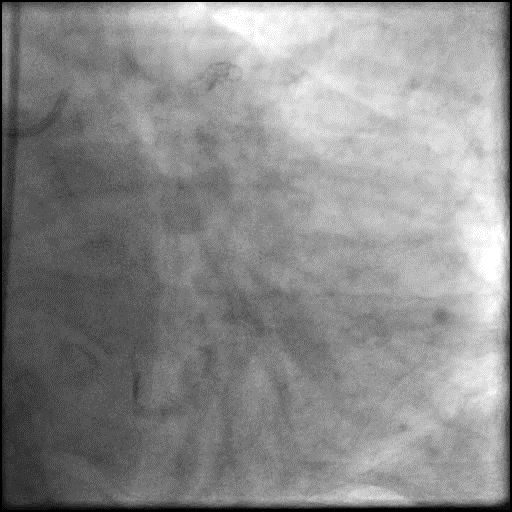
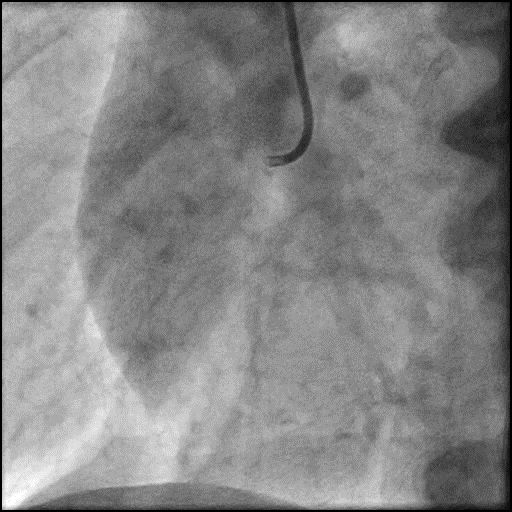
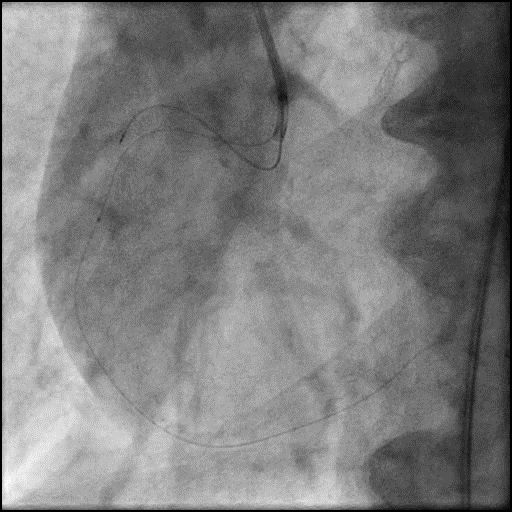
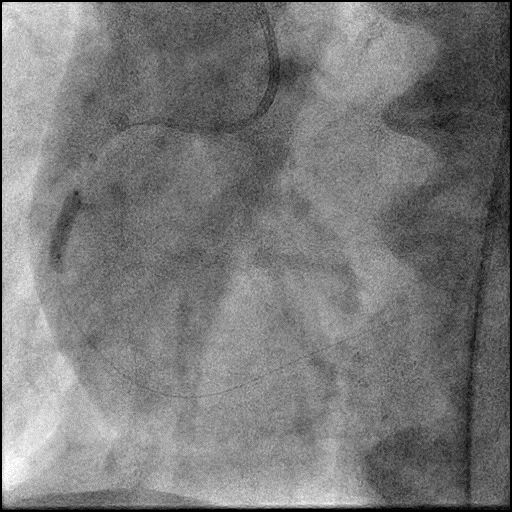
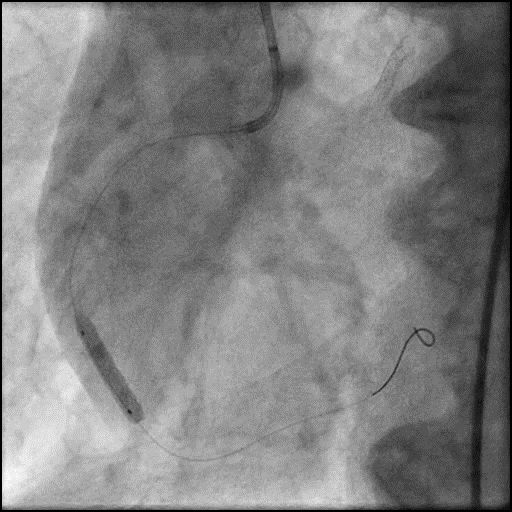
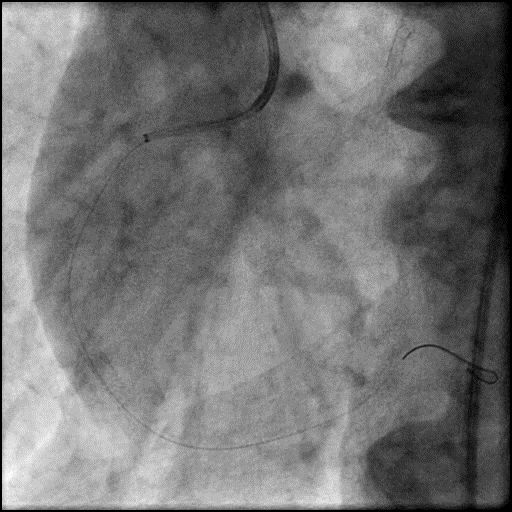
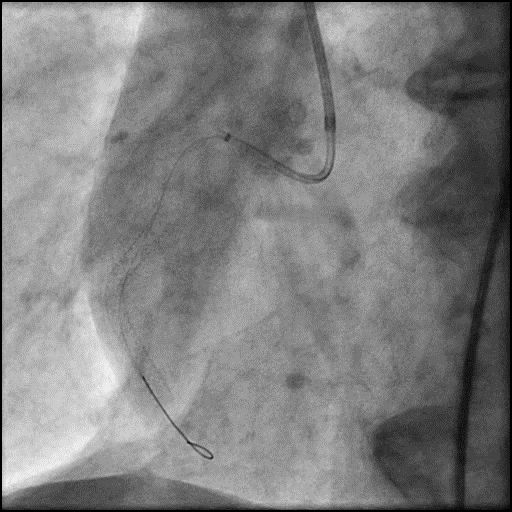
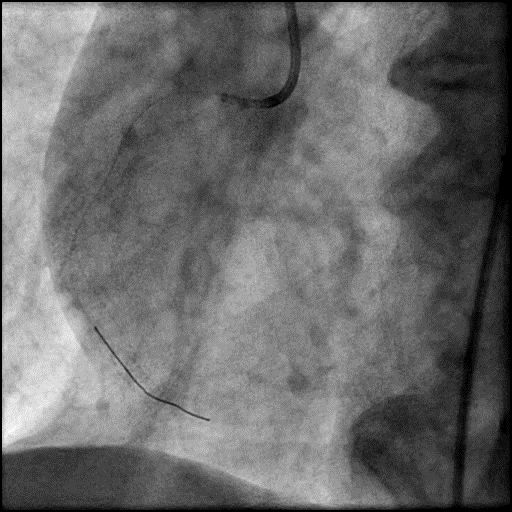
Angiograms
Post-procedure EKG
Case Overview
- Underwent intervention of the RCA.
- Procedure was complicated by slow flow following placement of a RCA stent.
- IC vasodilators were administered through the guide catheter without improvement in flow.
- Subsequently, IC vasodilators were administered to the distal vessel/microvasculature using a dual lumen microcatheter (Twinpass), successfully restoring flow (TIMI 2).
- Patient remained hemodynamically unstable with refractory chest pain; therefore, an IABP was placed.
- Troponin-I peaked at 71.7 ng/mL and CK-MB peaked at 344.9 ng/mL.
- Patient was discharged 3 days later without further sequelae.
Learning Objectives
- What is the likely explanation or reason why the complication occurred?
- Slow flow following stent placement – likely due to distal embolization of debris or thrombi.
- How could the complication have been prevented?
- Vasodilators should always be given prophylactically and for treatment of slow flow/no-reflow.
- Assure patient is given adequate periprocedure antithrombotic therapy (antiplatelets and anticoagulants).
- Pay close attention to the ACT during the procedure and dose anticoagulation accordingly to maintain ACT >300 prior to performing an intervention (Hemochron machine).
- We recommend using a intra-coronary imaging (OCT/IVUS) when performing an intervention involving an ectatic vessel.
- Intra-coronary imaging would have been helpful in delineating the composition of the plaque. If there was high burden of necrosis within the core of the plaque, this would have suggested the lesion is more prone to embolization if intervened on.
- Intra-coronary imaging helps determine the optimal stent length and diameter. This is important because in severely diffused ectatic vessels, the diameter and lesion length can be overestimated or underestimated.
- In diseased and ectatic vessels, intervention using a focal stenting strategy (with placement of a short and an appropriately sized stent) is preferred to reduce risk of slow flow/no-reflow.
- Of note, slow flow/no-reflow can still occur when using a focal stenting strategy, as was seen in this case.
- A stent should be sized one to one, and high pressure inflation should be avoided to prevent a “cheese-grater” effect in lesions which are prone to result in distal embolization.
- Is there an alternate strategy that could have been used to manage the complication?
- The initial step in management of slow flow/no-reflow involves administration of intra-coronary vasodilators through the guide catheter. If this fails, recommended using a dual-lumen microcatheter (Twinpass is the only dual lumen microcatheter available in the USA) to deliver intra-coronary medications to the distal vessel and microvasculature. Next, perform angiography with delivery of contrast through the microcatheter to determine if there is distal coronary flow. If distal vessel flow is not preserved the likely etiology of abrupt vessel closure (AVC) is no-reflow due to distal embolization of debris or thrombus, and IC vasodilators should be administered through the microcatheter targeted to the distal vessel and microvasculature. If flow is preserved, then the likely etiology of AVC is dissection (proximal to the point of microcatheter injection), and treatment involves placement of a stent. It is reasonable to perform aspiration thrombectomy prior to microcatheter based angiography injection (depending on the clinical context/presence of thrombus).
- Potent parenteral antiplatelet therapy should be employed when there is an acute stent thrombosis, which includes glycoprotein IIb/III inhibitor and/or IV cangrelor administration.
- What are the important learning points?
- The best treatment for slow flow/no-reflow is to prevent it from happening.
- The exact mechanism of the no-reflow phenomenon is unclear, but it is thought to be associated with endothelial swelling, neutrophil infiltration, and platelet aggregation causing obstruction and spasm in the microvasculature.
- Important to have multiple vasodilators readily available during a procedure. We use the following agents and administer them intra-coronary.
- Nitroprusside 50-200 mcg, Adenosine 30-40 mcg, Verapamil 100-200 mcg, Nicardipine 100-200 mcg
- Nitroglycerin 100-200 mcg (we use NTG for slow flow/no-reflow when it involved the epicardial vessels and not the coronary microvasculature)
- If the patient is hypotensive and this impedes the administration of intra-coronary vasodilators to treat slow flow/no-reflow, we recommend administration of IV phenylephrine 100-200 mcg as needed (may result in reflex bradycardia) to increase blood pressure, and then administer intra-coronary vasodilators.
- If there is refractory slow flow/no reflow then consider placement of an IABP. This helps with reduction in afterload, and improves coronary perfusion pressure by increasing coronary blood flow during diastole, and reduction in LVEDP.
- Depending on the size and function of the LV (LVEF <30%), consider using upfront LV support as it can help improve coronary perfusion pressure.
- Distal flow should always be established before placing a stent, unless dissection is considered as an etiology.