OCT Guided Left Main PCI
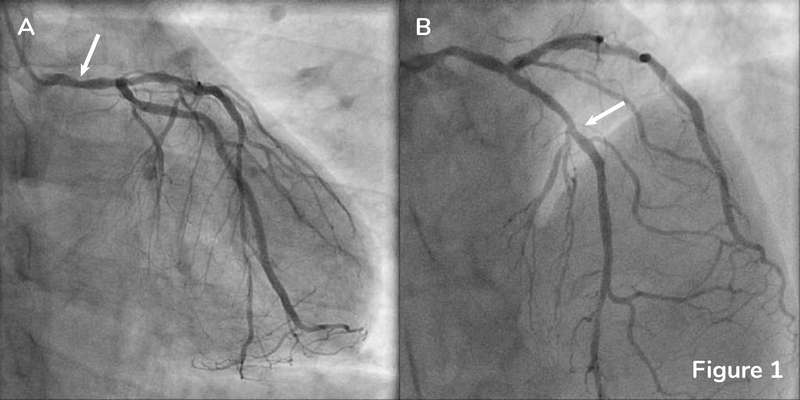
A 68-year-old man with a history of hypertension, diabetes mellitus, hyperlipidemia, and prior myocardial infarction two month prior presented with worsening angina and shortness of breath. Coronary angiography demonstrated a 70-80% lesion in the mid LM (Figure 1A) and 50-60% lesion in the proximal LAD with a patent DES in the mid LAD (Figure 1B).
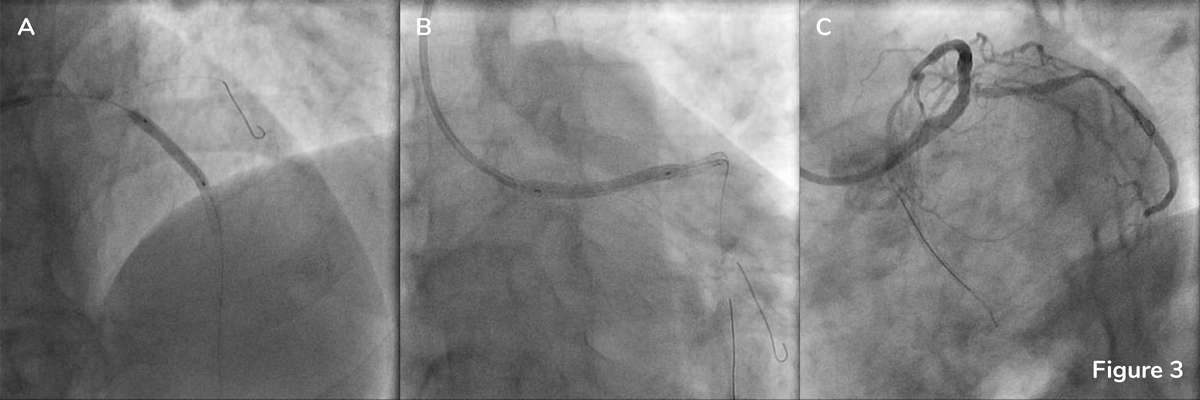
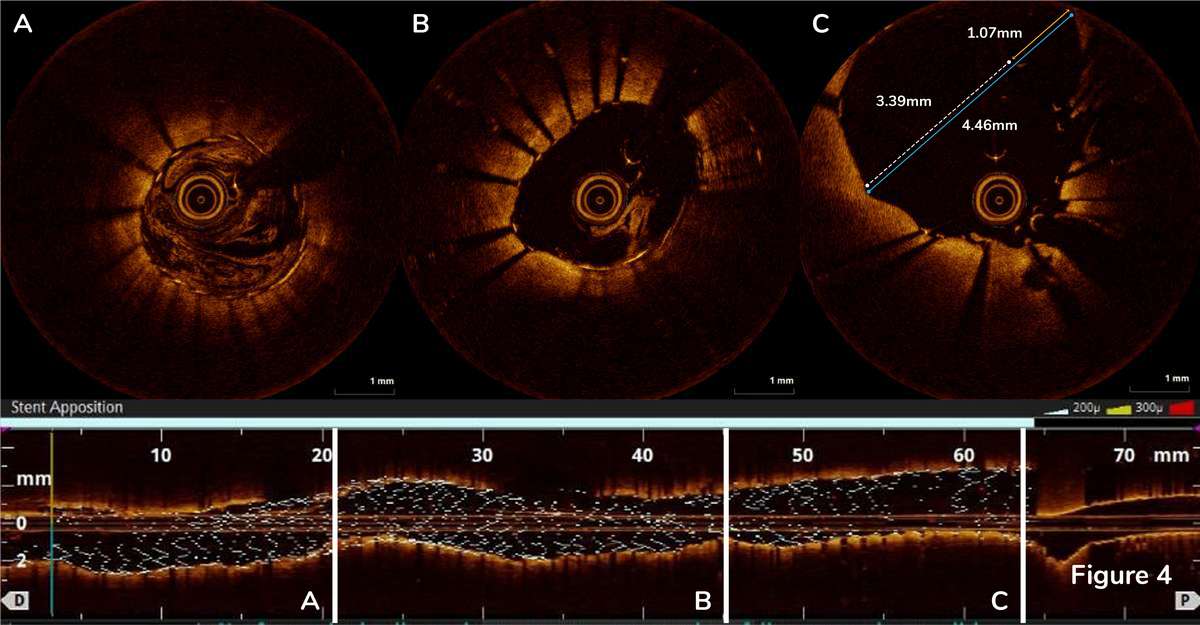
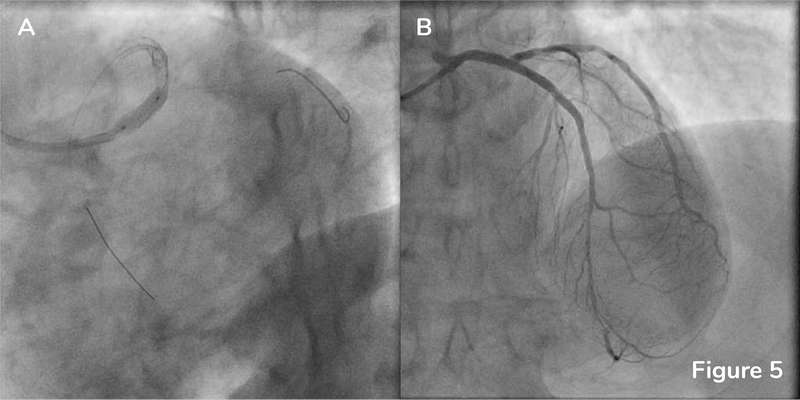
Post-stent OCT was performed without complete cannulation of the catheter in intention to assess the apposition of the stent deployed over the LM ostium. OCT confirmed optimal stent expansion and apposition in the proximal LAD with MSA 5.5mm2 (Figure 4A, there is residual blood in the vessel, however, stent struts can be clearly visualized) and LAD ostium (Figure 4B, small amount of residual blood is present in the cross section). Stent strut malapposition was detected by OCT in the proximal stent edge of the LM stent (Figure 4C) leading to a decision to perform post-dilatation with 4.5×15 mm NC EmergeTM Balloon (Figure 5A). Final angiography is shown in Figure 5B.
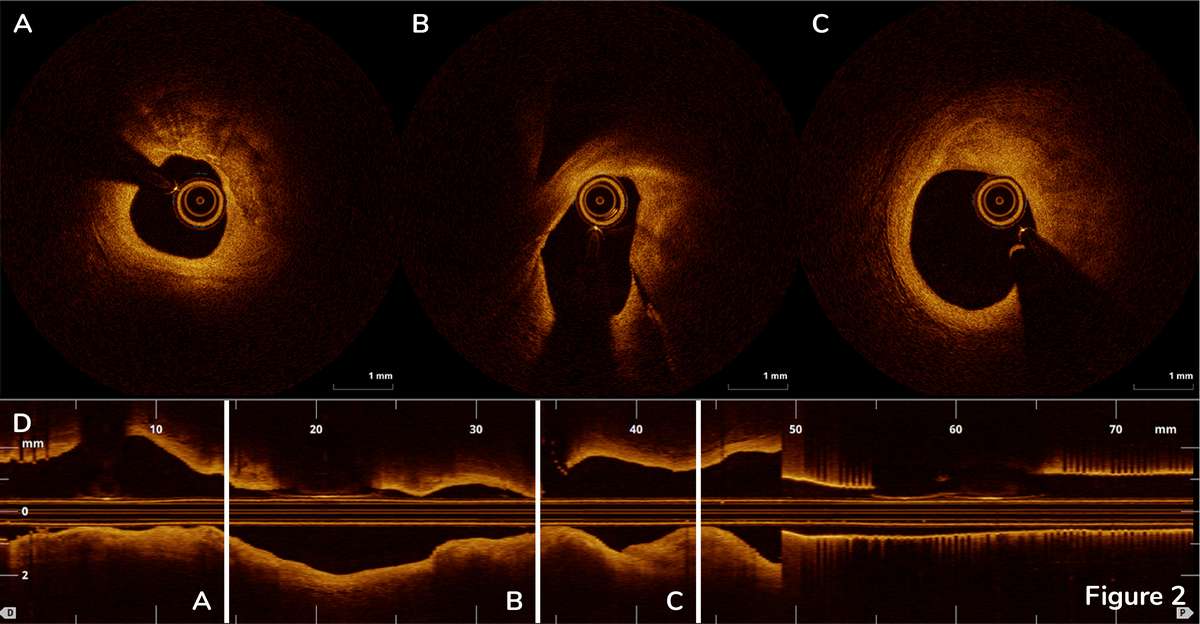
Displacement of arterial blood from the vessel lumen is required for OCT imaging, since the wavelength of OCT is shorter than red blood cell diameter. Blood clearance can be challenging in large vessels, such as the left main coronary artery, and in aorto-ostial lesions.1 In this case, we were able to successfully visualize aorto-ostial junction using OCT.
- IVUS-Guided Versus OCT-Guided Coronary Stent Implantation: A Critical Appraisal. JACC Cardiovasc Imaging. 2017;10:1487-1503