Pseudo-Stenosis/Accordion Effect – Case 1
Clinical Presentation
- 63-year-old female who presented with chest pain (CCS Class II).
Past Medical History
- HTN, HLD, Former Tobacco Use
- LVEF 65%
Clinical Variables
- Stress MPI: Small area of mild anterior ischemia.
Medications
- Home Medications: Aspirin, Atorvastatin, Isosorbide Mononitrate, Losartan
- Adjunct Pharmacotherapy: Clopidogrel, Ticagrelor, Heparin IV
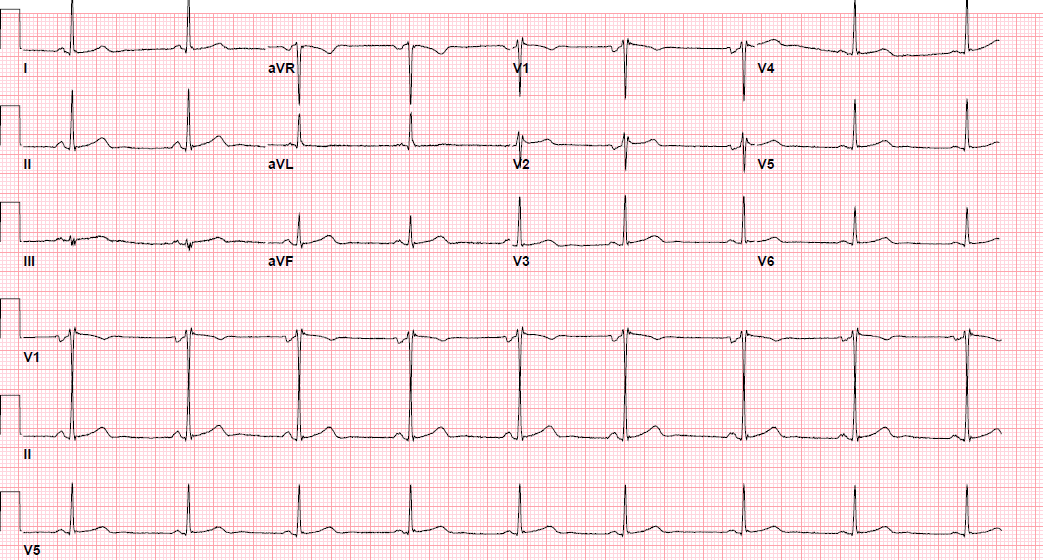
Pre-procedure EKG
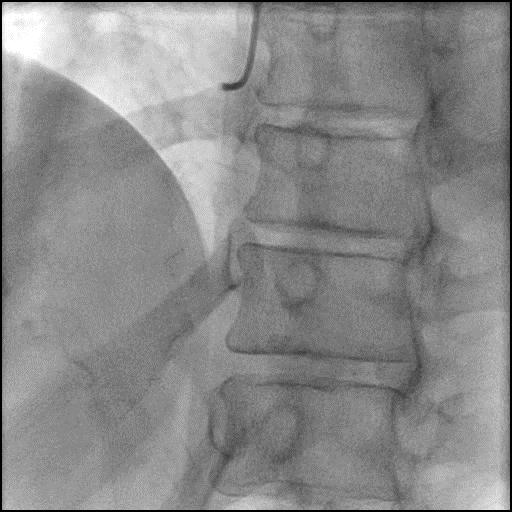
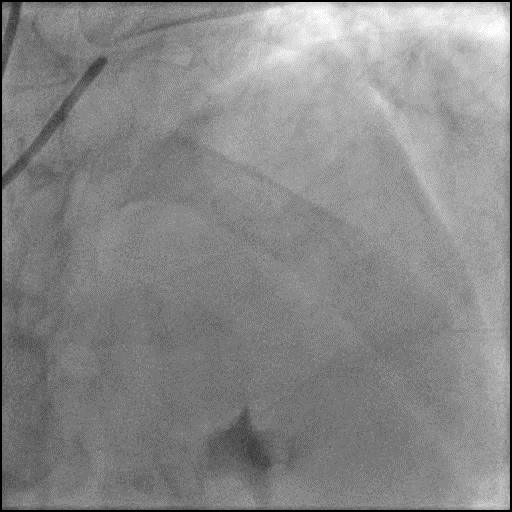
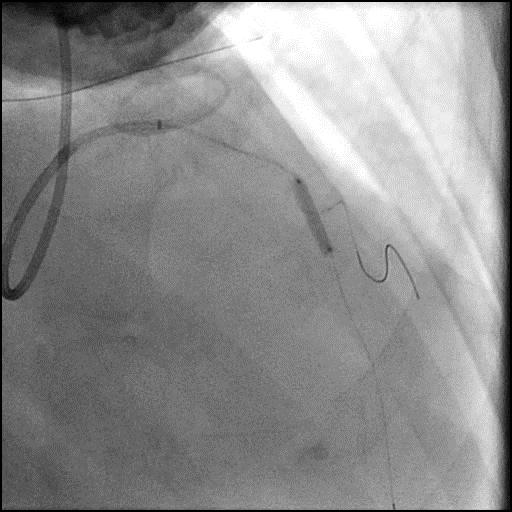
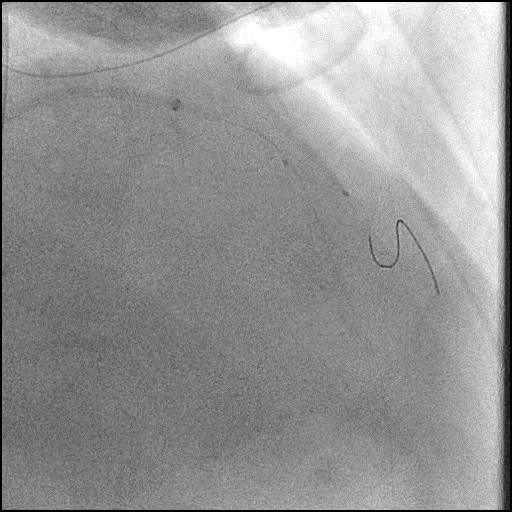
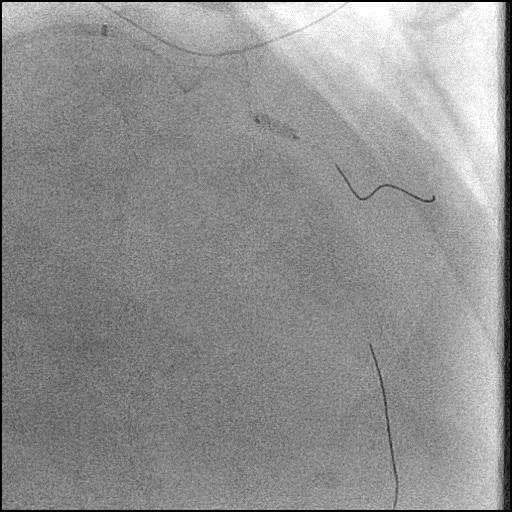
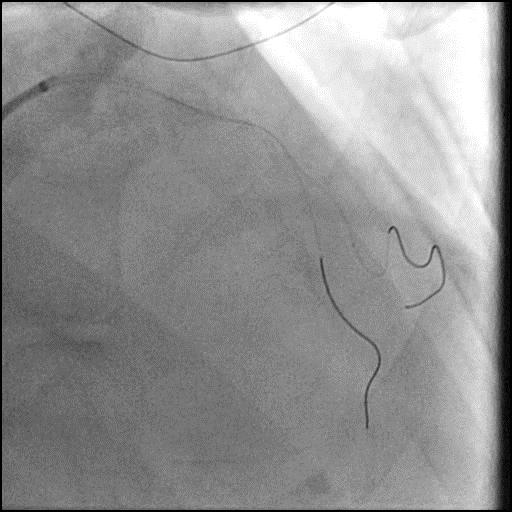
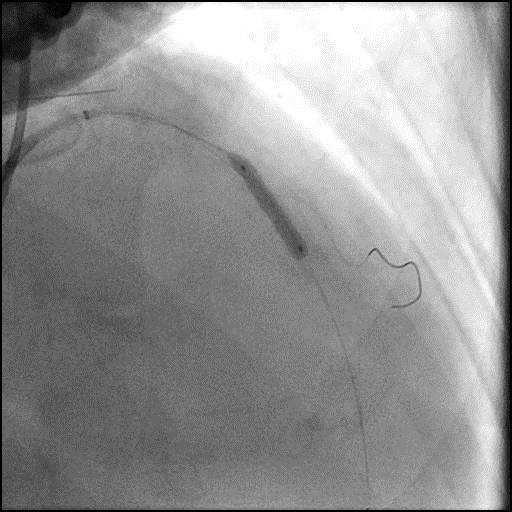
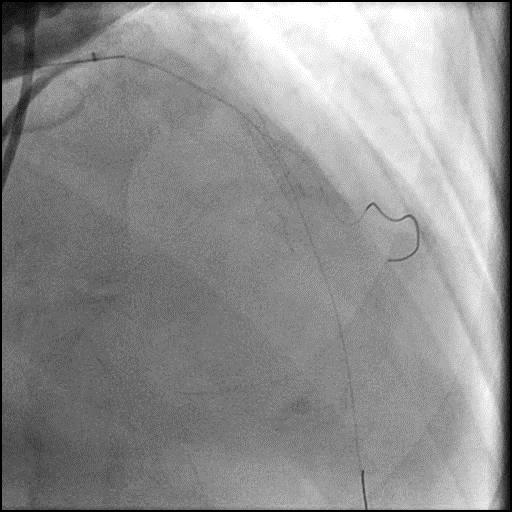
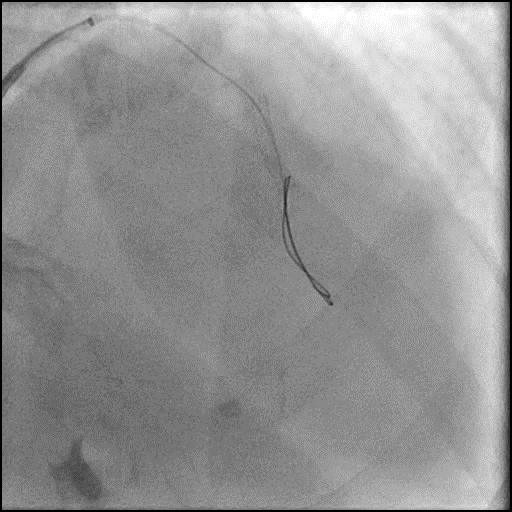
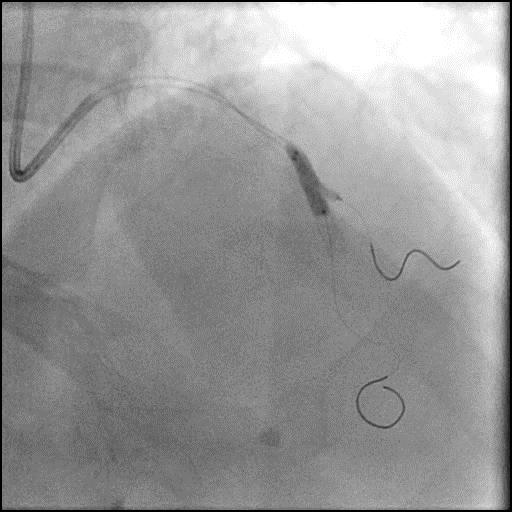
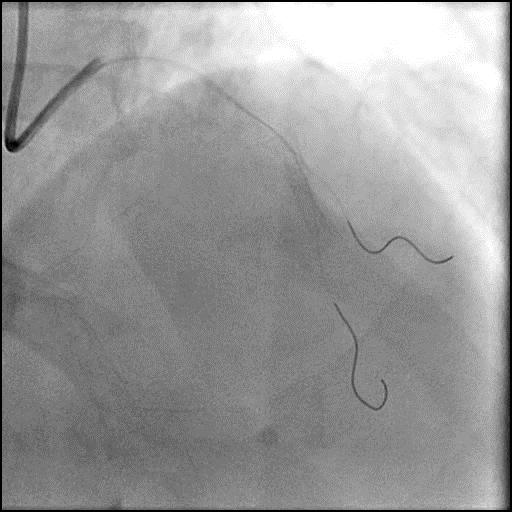
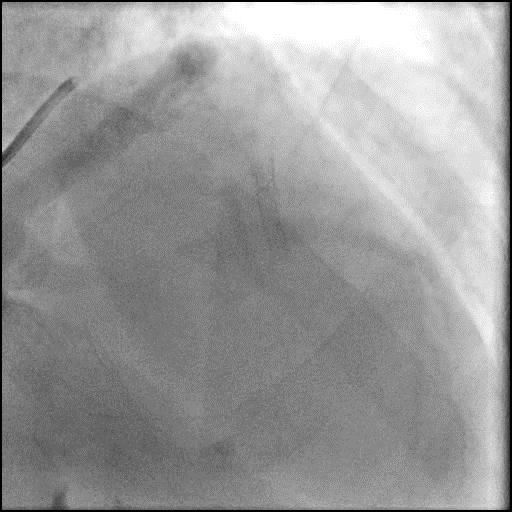
Angiograms
Post-procedure EKG
Case Overview
- Underwent intervention of the mid LAD-D2 bifurcation.
- After a stent was placed in the mid LAD, a new focal lesion proximal to the stent appeared.
- IC vasodilators were given with persistence of the focal lesion.
- The procedure was continued and after the wire was removed, the defect was no longer present, confirming the defect was likely due to a pseudo-stenosis.
- Troponin-I peaked at 0.22 ng/mL and CK-MB peaked at 2.1 ng/mL.
- Patient was discharged home the next day without further sequelae.
Learning Objectives
- What is the likely explanation or reason why the complication occurred?
- Pseduo-stenosis is also known as accordion effect and concertina phenomenon. It occurs when coronary equipment (i.e. coronary guidewire, stent etc.) causes mechanical distortion (folding/pleating) of a coronary artery along its long axis, and it presents as a filling defect.
- How could the complication have been prevented?
- Use a less supportive/stiff coronary guidewire.
- Is there an alternate strategy that could have been used to manage the complication?
- Intracoronary imaging (IVUS/OCT) may be helpful in elucidating the etiology of a focal lesion.
- It is reasonable and safer to diagnose pseudo-stenosis while leaving a guidewire within the coronary artery, and withdrawing it gradually until its radio-opaque (floppy) segment rests equally on either side of the suspect lesion. However, this technique is usually not feasible when there are multiple discreet lesions.
- If above technique fails, focal defect is located in the distal segment of a large vessel, reduced coronary flow with ongoing chest pain and EKG changes, or if there are multiple discreet lesions, then use a transit exchange catheter to remove the coronary guidewire. Place the exchange catheter distally over the guidewire and the remove the guidewire. This usually allows the vessel to return to its natural contour, resolving the pseudo-stenosis. It is important to position the exchange catheter distal as possible before removing the coronary guidewire because once the wire is removed, the vessel tortuosity will be restored and some position will be lost when reintroducing the wire. The guidewire can be exchanged, for a less supportive wire that will better conform to the artery contour if needed.
- What are the important learning points?
- If a new lesion appears while performing a procedure an operator has to consider a broad differential which includes coronary spasm, thrombus, dissection, plaque shift, and pseudo-stenosis.
- If there is a new focal lesion after introduction of coronary equipment, remember to review the initial acquisitions and administer IC vasodilators. Often times both a spasm and pseudo-stenosis can present simultaneously, and both IC vasodilators and removal of coronary equipment is necessary for the filling defect to resolve. It is essential to not lose wire position if there is concern for dissection or thrombus as being the cause of a filling defect.
- Recognition of pseudo-stenosis, is critical to prevent unnecessary interventions as it is only a transient angiographic filling defect that usually resolves with removal of coronary equipment.