Case 5: IVUS-guided PCI in ACS
Case Presentation
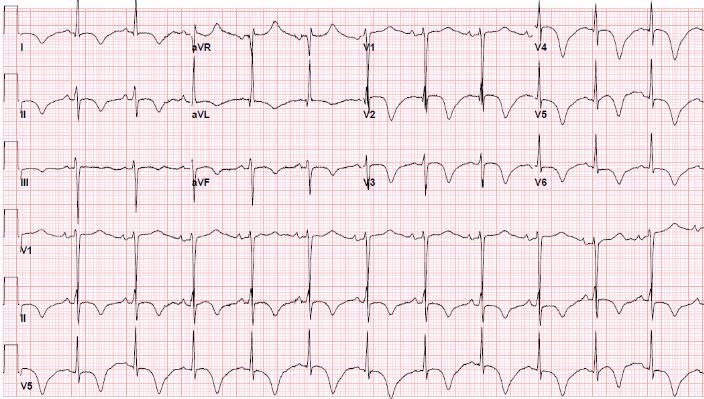
A 65-year-old male with CCS Class IV chest pain, elevated troponin with peak of 1.5 ng/mL, and EKG with massive anterior T wave inversions transferred from OSH to our hospital. He has initially presented with shortness of breath, chest pressure and progressed to respiratory failure requiring intubation and mechanical ventilation due to volume overload and CHF exacerbation. Echocardiography showed reduced left ventricular wall motion with ejection fraction of 25%.
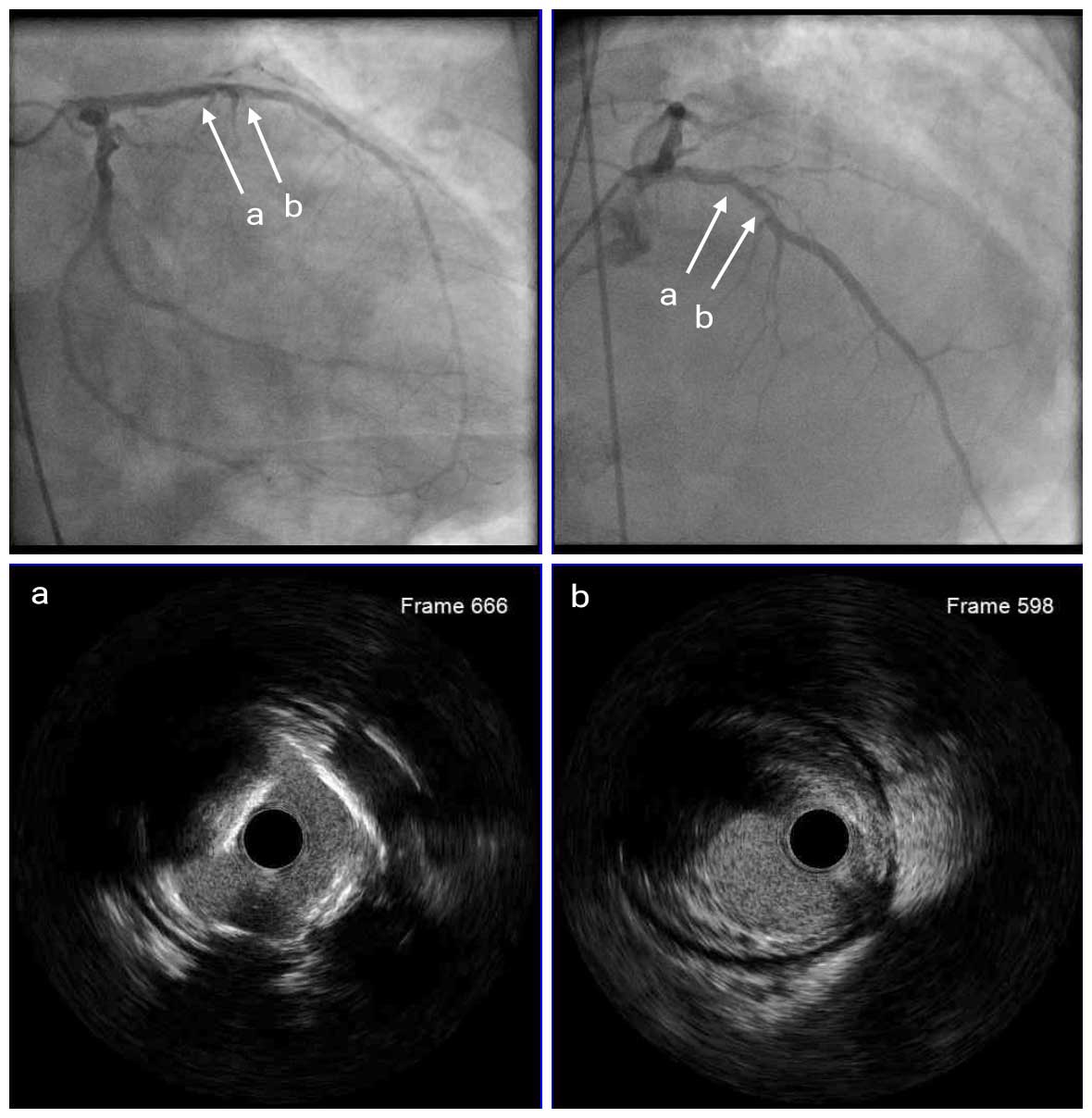
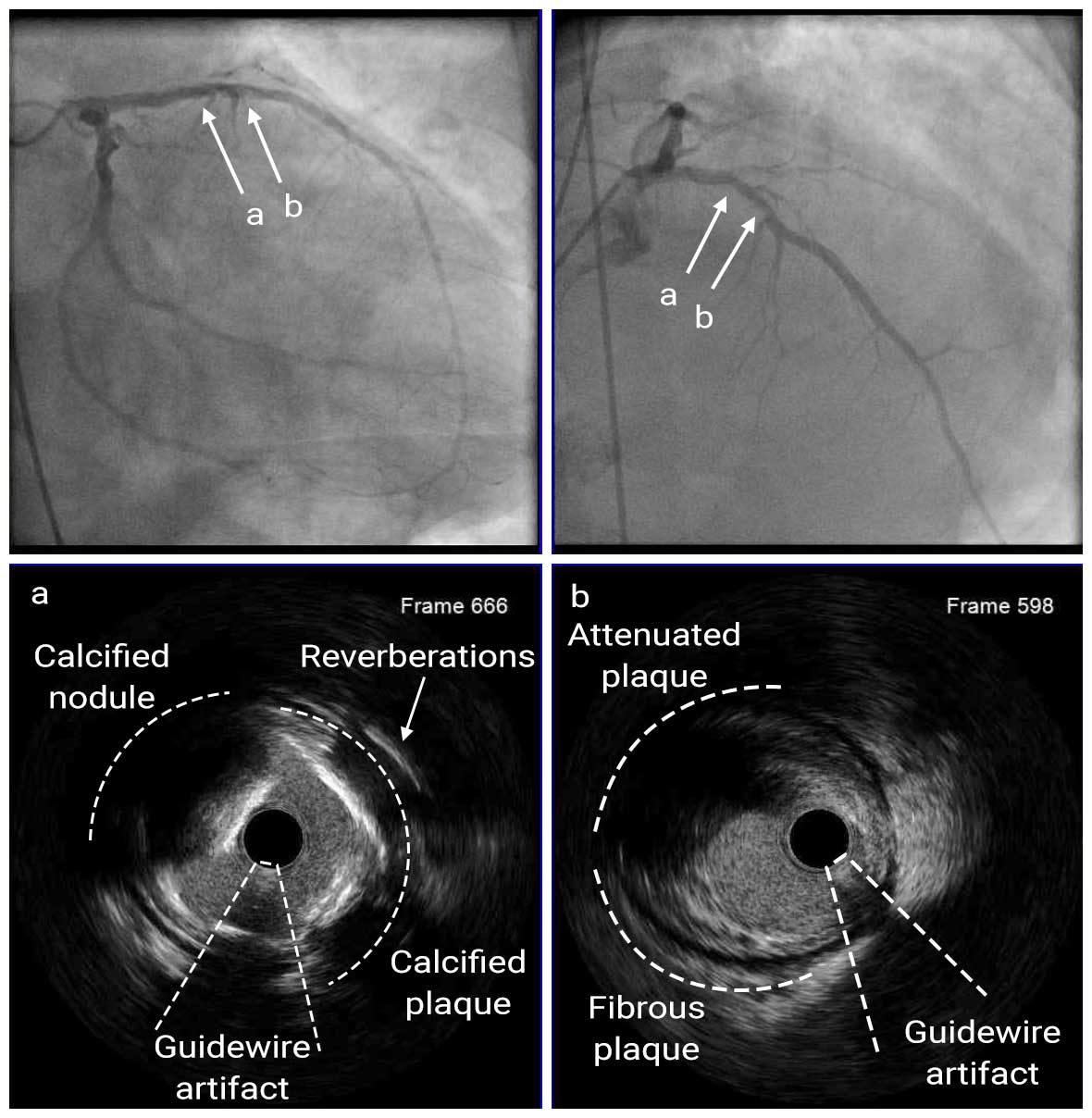
Although emergency coronary angiography showed no significant stenosis in the RCA, there was densely calcified 60-70% stenosis at the proximal LAD. Further assessment with IVUS showed attenuated plaque distal to a calcified lesion, which was identified as the culprit lesion and underwent PCI.
Pre Angio
Pre LAD IVUS
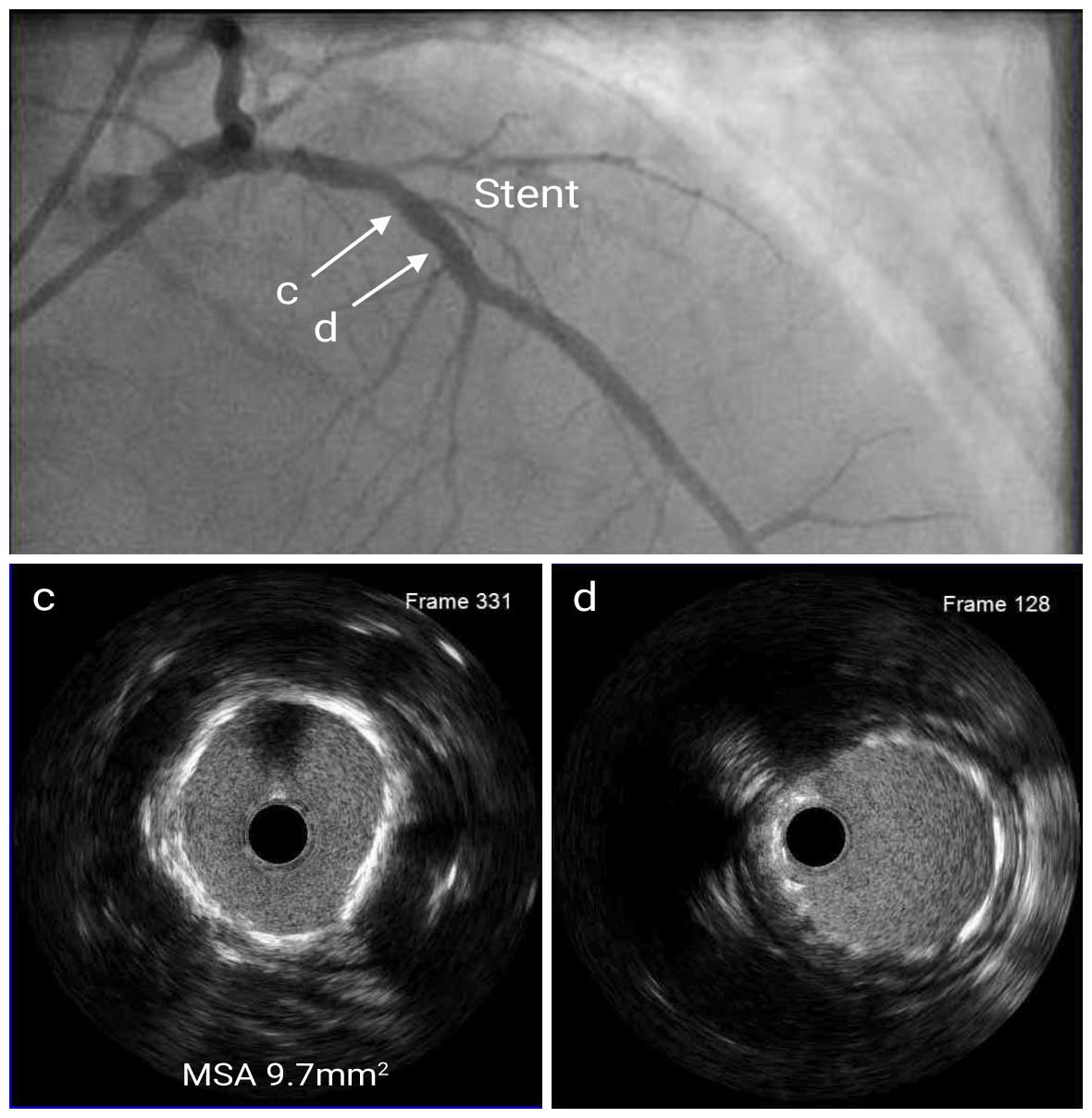
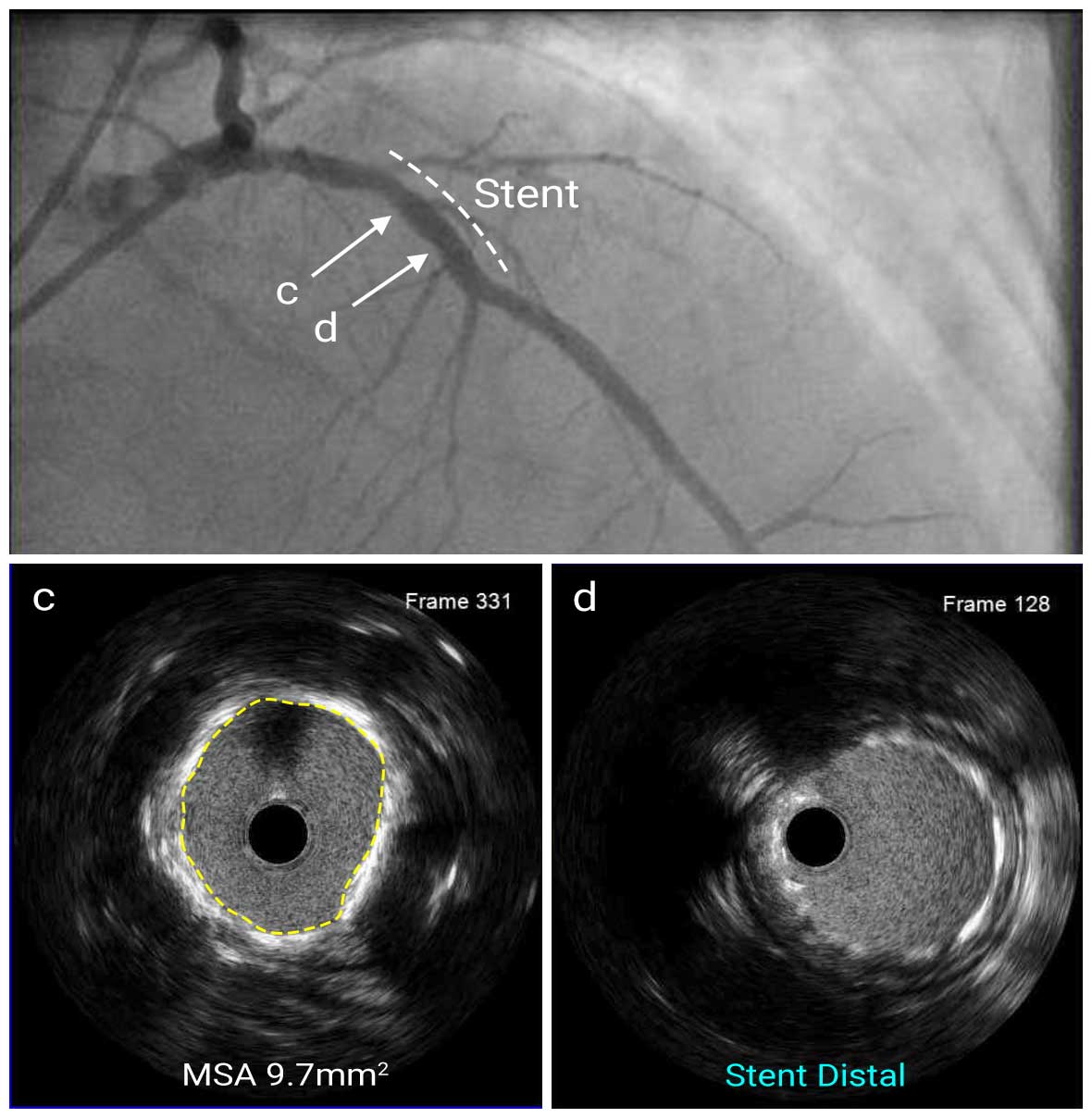
First, the lesion was pre-dilated with a 3.0mm scoring balloon and a 3.5mm non-compliant balloon up to 15 atm pressure. Then a 4.0mm x 12mm DES was deployed at the proximal LAD. The stent was post-dilated with a 4.0mm NC balloon up to 18 atm pressure. Post-stent IVUS showed good stent expansion (MSA=9.7mm2) and apposition without stent edge dissection.
Post LAD IVUS
Post Angio
In acute coronary syndrome, IVUS enables more accurate and detailed in vivo visualization of the culprit lesion compared to angiography. In this case, a thrombus was suspected in the proximal LAD due to hazy appearance on angiography, but IVUS identified calcification and an attenuated plaque.