Classification
Medina Classification
- Medina Classification is the simplest and most commonly used
- Indicates the location of significant stenosis (>50%)in the bifurcation
- This system classifies lesions into seven categories using a 3 component binary key based on visual assessment of lesion severity employing ≥ 50% stenosis as threshold
- Stenosis ≥ 50% is assigned a 1 for each of the three arterial segments of the bifurcation in the following order, proximal main vessel (pMV), distal main vessel (dMV), and side branch (SB)
- We did not include bifurcation angles into consideration while determining the interventional strategy since it’s not our routine practice
1.1.1
1.1.0
1.0.1
0.1.1
1.0.0
0.1.0
0.0.1
Guide size
Guide Sizes
- 7F system: For most two stent strategies including mini crush, V stent technique and SKS technique
- 6F system: For provisional stenting strategy , DK crush and coulette technique
Guidewire selection
Guidewire Selection
- Main Branch: Workhorse wires like BMW, Runthrough, ASAHI Sion, ASAHI Prowater
- Side Branch: Polymer coated (can be jailed; easy to recross) like Fielder, Hi-Torque Whisper
- Wire the challenging vessel first
- Shaping guidewire tip: To start, shape the wire tip in a J-shape or at a sharper angle. However, in many cases, the tip curve needs to be reshaped according to the side branch takeoff angle and tortuosity. Considering the variety of anatomical settings, our best recommendation is to adapt the length and angulation of the tip curve to the given anatomy
- According to the bifurcation angle, the guidewire can be shaped in 3 ways [see figure]
Stent size
Stent Sizes
- New generation DES is recommended
- Size Dilemma: If the main vessel stent is chosen according to proximal vessel (pMV) size there is a risk of distal stent edge dissection and carinal shift which can compromise the side branch. On the contrary, if the main vessel stent is chosen according to distal vessel (dMV) size there is a risk of stent malapposition at pMV site which can lead to stent thrombosis or cause difficulty in guidewire exchange.
- We therefore recommend choosing the stent size according to dMV and its expansion proximally to pMV size by either the final kissing balloon (2 stent strategy) or by proximal optimization technique (for provisional stent strategy)
Eg 1. Proximal Vessel 3.5mm in diameter and distal vessel 2.5mm in diameter- consider 2.75mm stent, deploy it at 10-12 atm and POT the proximal vessel with a 3.5mm short balloon at 16-18 atm
Eg 2. Proximal Vessel 3.5mm in diameter and distal vessel 3mm in diameter – consider a 3mm stent, deploy it at 10-12 atm, and POT the proximal vessel with a 3.5mm short balloon at 16-18 atm
Side branch should be rewired before performing kissing balloon inflation or proximal optimization technique (POT)
Balloon size
Balloon Sizes
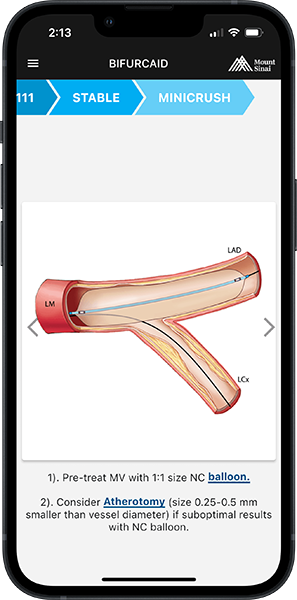
- For Predilation of SB: Non-compliant (NC) balloon sized typically 1:1 to vessel size
- If unable to cross with NC balloon, change to smaller diameter compliant balloon (e.g. 2.0/12 mm balloon)
- For Predilation of MB: Non-compliant balloon size typically 1:1 to vessel size
- If unable to cross with NC balloon, change to smaller diameter compliant balloon (e.g. 2.0/12 mm balloon)
- Atherotomy:
- Consider atherotomy of MV or SB if suboptimal results with NC / compliant balloon
- If SB has >70% stenosis and atherotomy balloon is available, consider atherotomy as first line treatment
- Size of atherotomy balloon is usually 0.25 to 0.5 mm smaller than vessel size
- If initial attempt of atherotomy resulted in suboptimal lesion preparation, consider upgrading the atherotomy balloon to 1:1 sizing
- For heavily calcified lesions or with suboptimal results with NC balloon or atherotomy, consider using atherectomy devices such as rotational atherectomy or orbital atherectomy
Provisional Stent Strategy
Provisional Stenting
- Provisional stenting is the strategy of placing a stent upfront in the main vessel only, and then reassessing the side branch for further treatment
- Considered when side branch < 2.5mm, has short lesion length < 10mm, has favorable bifurcation angle and in patients with medication compliance issues
Proximal Optimization Technique (POT)
POT
- POT is the technique of post dilating the proximal portion of the stent in the main vessel. The post dilatation is done with a short balloon either 1:1 in size or 0.5 mm more than that of the main vessel stent. The balloon for proximal optimization is kept in such a way that the distal marker is at the level of the bifurcation (by using a short balloon).
- This leads to:
- Strut expansion and stent apposition in the proximal main vessel
- Reconstruction of bifurcation anatomy and reducing the risk of side branch compromise related to shifting of the carina
- Facilitates side branch access after main vessel stent implantation
Kissing Balloon Inflation (KBI)
KBI
- Left Main Bifurcation KBI
- Both MV and SB balloons should be sized 1:1
- Non Left Main Bifurcation KBI
- MV balloon should be sized 1:1 and SB balloon is undersized by 0.5mm
These steps are common to both Left Main and Non Left Main Bifurcations
- If SB is difficult to recross, trying using a smaller size compliant balloon
- Short balloons are recommended over longer ones to facilitate recrossing
- First, sequential inflations are performed by inflating SB balloon at 16-18atm followed by MV balloon at a similar high atmospheric pressure. Then, align the proximal dots of MV and SB balloons and perform simultaneous kissing inflations and deflations of SB and MV balloons at lower atmospheric pressures
- If during kissing balloon inflation the balloon slips, consider doing sequential inflations with low pressures in the SB and high pressures in the MV
- Kissing balloon inflation reduces side branch thrombosis
Side Branch PTCA or Stenting During MV Provisional Stenting Strategy
Side Branch PTCA
- SB flow impairment (TIMI flow <3)
- SB dissection, chest pain or EKG changes
- Residual SB stenosis (a) LM > 50% and (b) non LM > 70% and SB is large enough to cause significant residual ischemia
- When future access SB may be important, e.g. during Left Main bifurcation to gain access into the circumflex branch or during non left main bifurcation when the side branch is a large caliber vessel
Bail out stenting technique
TAP (T-Stenting and Small Protrusion)
- If not already done, rewire SB through stent struts
- Pre-dilate SB with compliant balloon or NC balloon (preferred) at 14-16 atm to open up the MV stent strut
- Advance stent into SB
- Deliver uninflated NC balloon quarter size smaller in MV distal to SB
- Deliver SB stent, protruding 1-2mm in to MV
- Deploy SB stent
- Pull back SB balloon in to MV, realign the MV balloon, and then perform KBI
This technique provides coverage of SB ostium and creates a short neo-carina with minimal stent overlap in MV. Used when SB is smaller than MB. Major shortcoming of this technique is difficulty in accessing SB or MV in future.
Internal Crush / Reverse Crush
- Wire SB if not already done so or rewire SB through stent struts
- Dilate the stent struts of MV overlying SB using short compliant balloon [easier to recross] at high pressures (18-20atm)
- Deliver uninflated NC balloon quarter size smaller in MV distal to SB
- Deliver SB stent, protruding 2-3mm in to MV
- SB stent is deployed
- Remove SB wire and crush proximal edge of SB stent using NC balloon in MV
- Rewire SB through stent struts
- Perform final KBI
This is preferred bail out technique and is used when SB is smaller than MB.
Culotte
Two stent techniques
Two Stent Techniques
- SB diameter > 2.5 mm with > 50% stenosis in case of LM bifurcation and > 70% in case of non-LM bifurcation extending > 10mm beyond SB ostium
- Stent SB first
- Techniques: Mini crush, double kissing (DK) crush and Culotte
- SKS and V stenting are not routinely performed except in LM bifurcation as it creates double barrel in pMV
Types of Two Stent Techniques
SKS Stenting
- Wire MV and SB
- PTCA with NC balloon 1:1 size of both MV and SB. PTCA the branch with more severe disease first
- Consider Atherotomy with 0.25mm- 0.5mm smaller balloon if suboptimal results with NC balloons
- Advance SB stent first and then MV stent, sized to distal vessel
- Deploy both stent simultaneously at 10-12 atm
- Individual serial balloon inflation at 14-16atm
- Final KBI at 10-12 atm in both branches
Used with medina 1, 1, 1 disease and unstable patient. Carina during SKS stent technique extends to a considerable length (usually > 2 mm) into the main vessel
V Stenting: Steps similar to SKS technique. However, used in stable patients with Medina 0, 1, 1 disease i.e. LM not diseased. The stents in MV and SB are positioned such that there is minimal overlap in LM and proximal carina is < 2mm. If there is a plaque shift in to LM then consider Minicrush or DK crush.
Mini Crush
- Wire MV and SB
- Pretreat MV first and then SB with balloon 1:1 size
- Consider Atherotomy with 0.25mm- 0.5mm smaller balloon if suboptimal results with NC balloons
- Advance stent in to SB first followed by MV stent with proximal marker of SB stent retracted in to MV by 1mm; proximal end of MV stent should be proximal to SB stent
- Deploy SB stent and check results with angiogram
- Retrieve SB wire
- Position MV stent and deploy MV stent crushing SB stent
- Rewire SB through stent struts
- Advance NC balloon 0.25mm- 0.5mm smaller than SB stent diameter through SB ostium, if difficulty delivering NC balloon consider smaller compliant balloon
- Advance NC balloon 1:1 size in MV
- Serial post dilation at 16-18 atms, postdilate SB stent first
- Perform final KBI at 12-14 atms each
DK Crush
- Wire MV and SB
- Pretreat MV first and then SB with balloon 1:1 size
- Consider Atherotomy with 0.25mm- 0.5mm smaller balloon if suboptimal results with NC balloons
- Advance stent in to SB first retracted in to MV by 2-4mm
- Advance 1:1 size NC balloon in to distal MV
- Deploy SB stent and check results with angiogram
- Retrieve SB wire
- Position MV balloon and inflate crushing SB stent
- Rewire SB through stent struts
- Advance NC balloon 0.25mm- 0.5mm smaller than SB stent diameter through SB ostium, if difficulty delivering NC balloon consider smaller compliant balloon
- Advance back NC balloon in MV and perform first simultaneous kissing balloon inflation at 12-14 atm
- Remove both balloons and SB wire
- Advance MV stent and deploy and MV stent
- Rewire SB through crushed MV and SB stent struts
- Advance NC balloon sized 1:1 to distal vessel through SB ostium, if difficulty delivering balloon consider smaller compliant balloon
- Advance 1:1 size NC balloon in MV and perform second simultaneous kissing balloon inflation at 12-14 atm
Culotte
- Wire MV and SB
- Pretreat MV first and then SB with balloon 1:1 size
- Consider Atherotomy with 0.25mm- 0.5mm smaller balloon if suboptimal results with NC balloons
- First advance stent in to SB so that it extends in to MV to cover the lesion proximally
- Deploy SB stent and check results with angiogram
- Rewire MV through stent struts
- Advance NC balloon in to MV 1:1 size through stent, if difficulty delivering NC balloon consider smaller compliant balloon
- Balloon MV through SB stent strut to fully oppose proximal part of MV stent and create path to facilitate the stent in to MV
- Advance second stent in to MV leaving proximal overlap in the MV
- Remove SB wire prior to deploying MV stent
- Rewire the SB through crushed MV and SB stent struts
- Advance NC balloon 1:1 size in MV and SB
- Serial post dilation at 16-18 atms, postdilate SB stent first
- Perform final KBI at 12-14 atms each
Difficult SB Wiring Prior to MV Stent
Prior to MV Stent
- Use hydrophilic wire like Fielder, Whisper, Sion
- Pullback technique: Entering the SB by pulling back an angulated hydrophilic wire already inserted in the MB [see figure below]
- Reverse wiring technique- Similar to Pullback technique. Used when SB angle >130. First make a short (1-2 mm) acute angle bend (30-45°) at the tip, then add a second opposite bend at about 3 cm from the tip, choosing a rounded shape conformation (“swan-neck”). This bended guidewire is then inserted into the MV and manually steered back into the steeply angled SB.
- Consider plaque modification at carina with a smaller size balloon
- Consider using angled tip microcatheters like Venture and Supercross
Difficult SB Rewiring after MV stenting
After MV Stent
-
- Try using a new hydrophilic wire like Fielder, Whisper, Sion
- Use Balloon support to help redirect the wire
- Reshape the wire and use pullback technique
- Try swapping the wire from MV in to SB
- Consider repeating POT at higher pressure or with a bigger balloon
- Use angled tip microcatheters like Venture and Supercross if everything else fails
Inability to Pass Balloon in SB
Inability to Pass Balloon
- Use lowest profile balloon (1.00, 1.20 or 1.25 mm, 6-8 mm in length)
- Try Rewiring SB and make sure MV and SB wires are not tangled
- Try Accessing SB through a different stent strut
- Use POT to open struts of MB into SB
- Balloon anchoring technique: Inflate a balloon in MV distal to SB ostium at nominal pressure and then try deliver the balloon in to SB with MV balloon kept inflated. Deflate the MV balloon as soon as the SB balloon is crossed
- Use of microcatheters like Corsair, Turnpike, or Teleport (be cautious as it can damage MV stent strut)
Complications during Bifurcation Stenting
Complications
- Longitudinal Stent Deformation: A distortion of implanted coronary stent along its longitudinal axis during coronary intervention is known as longitudinal stent deformation (LSD). It occurs with guide catheter tip, balloons or use of other intracoronary devices like IVUS. It can lead to acute stent thrombosis and is managed by putting another stent at LSD site.
- Jailed SB Wire: After MV stent implantation, the SB wire can be trapped between the MV wall and the metallic structure of the stent. Difficulties in the removal of these wires can occur, and although extremely infrequent, the fracture of the jailed wire can also happen. Calcification of vessel wall, longer length of the trapped wire, and high pressure deployment of MV stent has been suggested as predictors of jailed wire fracture. It is imperative to use hydrophilic polymer coated wires in SB to avoid these complications.
- Distal edge dissection or perforation: Caused by vessel over stretching or due to presence of large, calcified, or attenuated plaques at the edges of the stent
- Our new complications website, ComplicAID, can be found here
Role of IVUS in Bifurcation Stenting
Role of IVUS
IVUS plays an important role in bifurcation stenting.
- For pre-procedure assessment of lesion severity and characteristics especially in left main lesions
- For pre-procedure assessment of lesion severity of the ostial left circumflex in cases where the ostium appears hazy or cannot be visualized well on angiography. If there is significant disease in ostial LCx then consider doing an upfront 2 stent technique.
- Post-PCI for optimization of results especially in left main stenting to make sure stent is well expanded and well opposed
Dual-Antiplatelet Therapy
Dual-Antiplatelet Therapy
- More potent antiplatelet therapies like Ticagrelor or Prasugrel can be considered in cases of two sent techniques
- In cases of Left Main PCI with 2 stent techniques, consider dual-antiplatelet therapy beyond 1 year